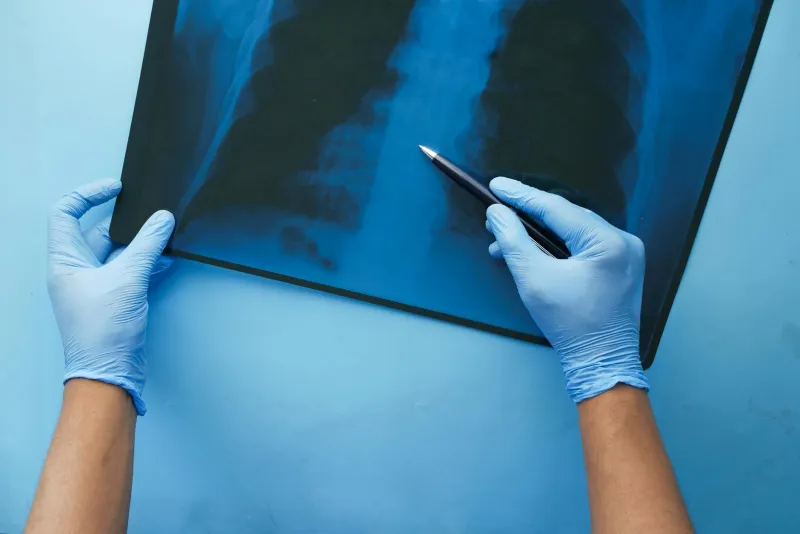
The Error That Started It All
Dr. Sarah Chen was having the kind of Tuesday that every radiologist dreads. It was March 1987, and she was three hours into reviewing a stack of routine chest X-rays at Regional Medical Center in Charleston, West Virginia, when she made what seemed like a catastrophic mistake.
 Photo: Regional Medical Center, via cdn.shopify.com
Photo: Regional Medical Center, via cdn.shopify.com
 Photo: Dr. Sarah Chen, via img.lb.wbmdstatic.com
Photo: Dr. Sarah Chen, via img.lb.wbmdstatic.com
The X-ray belonged to Marcus Webb, a 42-year-old coal miner from nearby Logan County who'd come in for his annual occupational health screening. Standard procedure, routine results expected. But something in the shadows of Webb's lung fields caught Chen's attention—a subtle scarring pattern that looked suspiciously like early-stage silicosis, the lung disease caused by inhaling silica dust.
There was just one problem: Webb worked in a coal mine, not a silica quarry. Coal miners got black lung disease, not silicosis. Chen had been reading chest X-rays for eight years, and she knew the difference. Or thought she did.
The Weight of Being Wrong
Chen flagged Webb's X-ray for follow-up testing, triggering a cascade of expensive procedures and workplace investigations. When the results came back negative for silicosis, Chen felt the familiar stomach-drop of professional humiliation. She'd been wrong, spectacularly and expensively wrong, and now everyone knew it.
Most doctors would have quietly filed the incident away as a learning experience and moved on. Chen couldn't let it go. "I kept staring at that X-ray," she later recalled. "The pattern was so clear to me, so obvious. But the tests said I was wrong, and tests don't lie. Except sometimes they do."
Instead of burying her mistake, Chen did something unusual: she started collecting similar cases. Every time she saw an X-ray with that same subtle scarring pattern—the pattern that "shouldn't" exist in coal miners—she documented it, filed it away, and quietly began building a database of anomalies.
The Pattern in the Shadows
What Chen discovered over the next eighteen months would challenge everything the medical community thought it knew about occupational lung disease. The scarring pattern she'd been seeing wasn't silicosis—it was something else entirely, something that existing diagnostic criteria weren't designed to catch.
Working with a small team of graduate students from West Virginia University, Chen began mapping the geographical distribution of these "mystery" X-rays. The results were startling: the cases clustered around specific mining operations, but not the ones anyone expected. The pattern didn't follow traditional coal seams or known silica deposits. Instead, it seemed to correlate with mines that had been using a particular type of sandstone as tunnel support material.
 Photo: West Virginia University, via i.pinimg.com
Photo: West Virginia University, via i.pinimg.com
Further investigation revealed the smoking gun: the sandstone contained crystalline silica, but in a form that was being released into mine air through a previously unknown mechanism. When the stone was subjected to the specific vibrational patterns of modern mining equipment, it created silica dust particles so fine they weren't being caught by standard air monitoring systems.
The Cover-Up That Wasn't
Chen's research revealed that miners across five states—West Virginia, Pennsylvania, Kentucky, Ohio, and Virginia—had been unknowingly exposed to this "stealth silica" for over a decade. The lung disease it caused looked different from classic silicosis on X-rays, developed more slowly, and was often misdiagnosed as coal workers' pneumoconiosis or even early emphysema.
More troubling still, Chen discovered that several mining companies had been aware of elevated silica readings in their air samples but had dismissed them as measurement errors because the levels didn't correlate with expected sources. The "errors" had been consistent across multiple mines and multiple years, but no one had connected the dots.
"It wasn't a conspiracy," Chen emphasized in her landmark 1990 paper. "It was something worse—a blind spot. Everyone was looking for the disease they knew how to find, so they missed the one that was actually there."
The Ripple Effect
Chen's findings forced a complete overhaul of occupational health protocols in the mining industry. New testing procedures were implemented, air monitoring systems were upgraded, and thousands of miners received medical screening for the previously unrecognized condition. The economic impact was enormous—mining companies faced hundreds of millions in liability costs and equipment upgrades.
But the human impact was more significant. Chen's willingness to investigate her "mistake" led to early detection and treatment for over 3,000 miners who would otherwise have faced progressive, irreversible lung damage. Her work also revolutionized how occupational medicine approaches diagnostic anomalies, establishing protocols for investigating "impossible" cases rather than dismissing them.
The Doctor Who Wouldn't Let Go
Today, Dr. Chen is considered a pioneer in occupational pulmonology, with her 1990 research paper cited in medical textbooks worldwide. But she's most proud of a different statistic: the mortality rate from mining-related lung disease in her region has dropped by 60% since her "mistake" led to new safety protocols.
"People ask me what made me keep digging when everyone said I was wrong," Chen reflects. "The truth is, I wasn't brave or visionary. I was just stubborn. I couldn't stand the idea that I'd made such an obvious error, so I kept looking for proof that I wasn't crazy."
Chen's story has become required reading in medical schools as an example of how scientific progress often comes from embracing uncertainty rather than avoiding it. Her "mistake" saved thousands of lives because she refused to accept that she could be so completely wrong about something she could see so clearly.
Sometimes the most important discoveries happen not when we get things right the first time, but when we're humble enough to investigate why we might have gotten them wrong. In Chen's case, one misread X-ray became the key that unlocked a medical mystery hiding in plain sight, proving that in science, as in life, our biggest failures often contain the seeds of our most important successes.